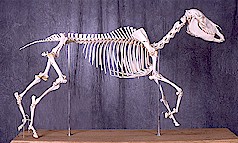
General Health II Your Horse's Bone Structure
Great Articles! Little Magic Shoes - Correction shoes for Minis - Must see! "HYPERLIPEMIA"...QUICK & DEADLY Recent events have prompted me to write this article as an "alert"
to all Miniature Horse owners about a very serious condition called "Hyperlipemia".
I had never heard of this particular malady until just a few months ago when a
couple of my friends had Minis come down with this, and came very close to
losing them! I have since read of many, many others on the internet who have had
experiences with the same condition...and in most cases, the Minis died! In this
day & age of e-mail, world-wide web, surfing the net, etc, etc...we are all
much more "connected" to people all over the country (not to mention
the world!) One lady who was experiencing Hyperlipemia with her Mini mare wanted
to learn more...and requested, on line, that others who had similar experiences
to please contact her. She was shocked at the number of responses she received.
36 Minis were affected (27 mares & 9 colts/stallions). 13 lived....23 DIED! . . BUTE vs BANAMINE use in Minis Bute is incredibly toxic to minis, and for
some reason a lot of vets out there don't realize this. Not only is there a very
narrow safety margin, i.e. you have to be very accurate at dosing them, but
there are minis who will have problems even at the correct dose. It should be
given at 1mg per pound body weight, which means most minis will get 150 mg to
250 mg--1/4 tablet or less. A lot of vets seem to think the average mini weighs
500 pounds and have owners give 1/2 tablet twice daily. ARGGGG!!!
Quick Review of Horse Diseases Anthrax: Anthrax is a bacterial disease that varies in presentation with the mode of infection. Horses most commonly show septicemia, enteritis and colic. Anthrax is caused by the organism Bacillus anthracis. Distribution of the disease is worldwide, but it is not commonly reported in the United States. Vaccination is only recommended in enzootic areas of the country (i.e., South Dakota, Louisiana, Texas, Missouri, California, and Arkansas). Most cases of anthrax are reported during the warm summer months, but the disease may occur in the winter. In the case of an outbreak, only those animals not exhibiting clinical signs should be vaccinated. The equestrian should consult with their local veterinarian, as this is not a commonly given vaccine. Botulism: Botulism is a neuroparalytic disease caused by the organism Clostridium botulinum. It is geographically enzootic in some areas of the world. In North America, type B is most commonly found in the Mid-Atlantic States and Kentucky. Type A is prevalent west of the Rocky Mountains, and type C arises mainly in Florida. Most foals are infected via growth of the bacterium within the gastrointestinal tract (toxicoinfectious botulism) between two weeks and eight months of age. Affected foals are referred to as having "shaker foal syndrome." Adult horses are most commonly infected via ingestion of preformed toxins referred to as "forage poisoning." Clinically, horses develop a progressive muscle paralysis that affects the limbs, jaw and throat muscles, the upper eyelid, tongue, and tail. It should be noted that the vaccine only offers protection against type B. Enchephalomyetis: Encephalomyelitis is a viral disease of horses. The three types are eastern, western, and Venezuelan. Various neurologic signs, including excitement, dementia, head pressing, and circling, characterize the disease. Transmission occurs by vectors (i.e., mosquitoes), and the disease is generally associated with areas inhabited by these vectors and where winter temperatures are usually not severe. Vaccination before vector season and biannually in humid areas of the country is recommended. The vaccine for encephalomyelitis is often polyvalent in combination with tetanus toxoid, influenza, or other vaccines. It is important to note that vaccination with the Venezuelan type may interfere with exportation of horses to some European countries because of seroconversion. Equine Viral Arteritis: Equine viral arteritis is a viral disease caused by a arterivirus that can cause respiratory disease and abortion in horses. The vaccine is only recommended for use in stallions, open mares, and young horses six weeks of age or older. Pregnant mares and open mares or stallions that are within three weeks of being bred should not be vaccinated. Vaccination may interfere with exportation to some countries because of seroconversion. Before using the vaccine, veterinarians/horsemen should check with their state veterinarian because some states regulate its use. Influenza: Influenza is a viral disease that affects the upper respiratory tract of horses. Vaccination with a killed virus vaccine requires frequent administration (every two to six months) to provide appropriate protection to susceptible horses. A modified-live virus intranasal vaccine is also currently available. The vaccine is available in monovalent or polyvalent forms. A transient postvaccinal fever occurs in some horses. Other horses also may show a loss of appetite and depression after vaccination. Once a horse is infected, the upper respiratory tract takes three weeks after remission of the disease to recover fully. Thus, the significance of immunizing the competitive and/or show horse to prevent costly layoff is apparent. In addition, it is equally important to vaccinate horses traveling to and from sales and breeding farms. Current recommended vaccination schedules are every six months for adult horses at low to moderate risk and every one to three months for high-risk animals. Vaccinations should not be administered two to three weeks before a stressful event, such as a show, because of the increased chance of the previously mentioned side effects. Potomac Horse Fever: Potomac horse fever (equine monocytic ehrlichiosis) is caused by E. risticii. The disease is characterized by diarrhea, ileus, and often laminitis. The disease has been reported mainly in the northeastern United States and Canada but has occurred in other countries. The disease is seasonal and usually occurs in late spring to early fall. As soon as Potomac horse fever occurs on a farm, there is a high risk of recurrence. A freshwater snail is suspected to play a role in the transmission of the disease. Current vaccines offer short-term protection, and revaccination every six to twelve months is recommended. If an infected horse survives, it will maintain immunity for about two years, and should not require immediate revaccination. Vaccine failure has been reported in endemic areas. Rabies: Rabies is a rhabdovirus that causes neurologic disease. The disease can cause a large variation in clinical signs that range from lethargy to bizarre, frightening behavior. Horses in enzootic areas should be vaccinated, especially those exposed to wildlife. In some horses, a local tissue reaction occurs, and thus intramuscular vaccination is recommended in the lower thigh, not in the neck. Some vaccines of this type can be given subcutaneously (just under the skin). Vaccinated horses that are exposed to a rabid animal should be revaccinated and observed for 45 days. A licensed veterinarian should examine the horse at the initial time of injury and perform follow-up evaluations. Rabies is invariably fatal in unvaccinated horses, and it is zoonotic; therefore, unvaccinated horses exposed to a rabid animal should be euthanized. Vaccination of unvaccinated horses after exposure to the disease is not recommended. Owners unwilling to have their horse euthanized should isolate and closely observe the animal for six months. This isolation must occur under the authority of the rabies control agency. Illness or behavioral change must be reported the local rabies control agency immediately, and the horse must be evaluated by a veterinarian. If clinical signs are suggestive of rabies, euthanasia of the animal is required for rabies testing. Rhinopneumonitis: Rhinopneumonitis is a viral disease caused by the equine herpes virus. There are five herpesviruses that affect horses with an additional three that affect donkeys. Of these, two types cause the most significant disease. These are equine herpesvirus type 1 (EHV-1) and type 4 (EHV-4). Both of these cause the disease known as rhinopneumonitis. Three disease forms of the equine herpes virus infection may be identified: respiratory, abortion, and neurological. Of these, you can only vaccinate for the respiratory and abortion form of the disease. Vaccination is not 100% effective, and the neurological form of the disease cannot be vaccinated against. The vaccines currently licensed for use in horses offer short-term immunity and require frequent administration. Vaccination every two to three months is recommended, depending on the environmental risk. Pregnant mares that are in contact with mares that have recently aborted fetuses infected with EHV-1 should be vaccinated with one of the inactivated vaccines. This vaccination may produce immunity for those mares in the group that are not incubating an abortogenic infection at the time of vaccination. It is important to note that all rhinopneumonitis vaccines make no claim to prevent the neurologic form of the disease, and only two claim to prevent the abortion form of the disease. Horses do not develop immunity to the neurological and abortion forms of the disease; thus, the need for vaccinating our horses. The horseman should use a vaccine that contains both the EHV-1 & EHV-4 virus strains. Preventive medicine is best when the combined EHV-1 product is used (EHV-1 + EHV-1b). Pregnant mares should be vaccinated at five, seven, and nine months of gestation with vaccines approved for use in gestating horses. Strangles: Strangles is a highly contagious respiratory disease seen mainly in young horses and caused by Streptococcus equi. The disease causes swelling of the submaxillary, mandibular, and retropharyngeal lymph nodes (those under and between the jaw and in the throatlatch area). In severe cases, the extreme swelling of these lymph nodes causes the horse to sound as if it is being strangled, thus the origin of the name "strangles." Some horses have died due to asphyxiation caused by airway obstruction. Although abscesses mainly occur in the throatlatch region or between the jaws, they have also been reported in the chest, gastrointestinal tract, and other regions of the body. Other characteristics of the disease include acute fever, acute pharyngitis, and respiratory distress. Although morbidity is often much higher than mortality, the disease can cause immense distress to infected horses. Vaccination of horses is controversial. Currently, three intramuscular vaccines are available to the equestrian and all have been associated with post-vaccinal reaction or abscesses at the site of injection. It is therefore considered wise to vaccinate the horse in a low (easily drained) area of the body if one of these types is used. A modified-live intra-nasal vaccine offers excellent protection to the horse. This vaccine should be administered by your veterinarian, and protective disposable gloves must be worn when giving this vaccine. Bacterial particles from the vaccine may become distributed on the hands during administration. If giving another intramuscular shot to the horse, injection of the bacteria and a subsequent abscess may develop at the injection site if proper sanitary methods are not utilized. Outbreaks of the disease have been reported in horses vaccinated according to manufacturer's recommendations with all vaccines. The severity and duration of the disease, however, seems to be reduced by vaccination. In view of these possible problems, the advantages of vaccination must seriously be considered. Unless horses are presently in a high-risk environment, vaccination may not be warranted. High-risk environments include farms where strangles are enzootic or broodmare farms where horses of unknown disease/vaccination status come in contact with each other and resident farm animals. In these areas, broodmares should be vaccinated prior to breeding and three to six weeks before foaling and foals should be vaccinated at two to three months of age and again at six months of age. Depending on the environment and vaccine used, either an annual or biannual vaccination protocol can be practiced. . ~~~ BACK TO INFO MAIN PAGE ~~~ Get me back to Lil Beginnings Miniature Horses main page please! |